In an article from the American Sleep Association they recommend some of the basics to start with such as avoiding caffeine for several hours before bedtime. They report that brainwave patterns during can continue to show effects of a double espresso coffee 16 hours after it was consumed! In the same study, the measurable level of caffeine […]
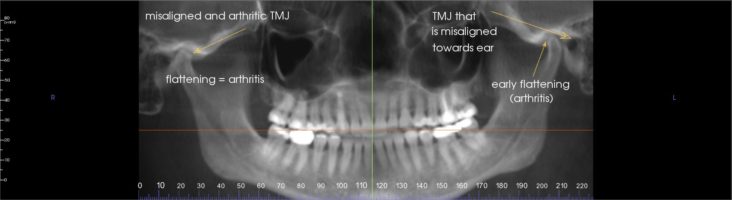
Can A Panorex Dental X-ray Detect TMJ Problems?
Yes and no. TMJ problems such as slipped discs (clicking or popping noises) or complete disc dislocation (can’t open your mouth very far) doesn’t always show up on radiographs until the condition has been going on for a few weeks, months or even years. Clicking, popping or locking of a jaw joint happens when the […]

Accutane, Bruxing and TMJ
Recently, a patient presented with “clicking” that has progressed to having a locked left jaw in the morning. They can “unlock” it easily at this point. The clicking symptoms started when they were taking Accutane for acne and the clicking seemed to resolve when Accutane was discontinued. Did Accutane have anything to do with this? […]

How It’s All Linked: The Facts
Let’s face it; what we all want is to spend quality time with those we love. We value health and happiness, experiencing life’s adventures, and snuggling in warm and cozy on a winter’s day. But the truth is most families experience health issues, questions arise and the unknown keeps us from living our lives the […]

The Many Questions of TMJ (and OSA)
Studes, recommendations, allies and liabilities all play a part in creating the information available when trying to get answers to the many questions surrounding TMJ. Some studies are designed to follow a single-symptom, linear progression protocols, which means the study is not able to follow a new symptom even if the change is of problem […]

Dehydration, Nighttime Urination, Bedwetting and How It Relates to Obstructive Sleep Apnea
Dehydrated? Get more sleep….Tired? Drink more water….it’s all connected. This article reviews what we already know about proper sleep time and quality: if your sleep is disrupted it affects our entire body chemistry. Kidney function is also impacted by Sleep Apnea and other sleep breathing problems. Proper length and depth of sleep is known to […]

The Impact of Cell Usage on College Kids
Research shows that use of electronics pre-bedtime can affect sleep. A recent study of college students’ use of Cell Phones after “lights out” was shown to definitively contribute to sleep disturbances and mental distress. This was a large, significant group of almost 4,400 college students self-reporting cell phone use and specifically, use in bed after […]

The TMJ Treatment Debate Debunked
If you search for advice with TMJ problems, some sites suggest simple self-care is all you should do. And they say it’s a “self-limiting muscle tension problem” that will resolve. Decades ago that might have been believed. With improved imaging technology, there is understanding of the progressive damage to the TMJ (one study showed nearly […]

You, The Well-Informed Parent: Advocate for Your Children and Teens!
In my last post, it was my intention to pay attention to how your children are sleeping (or not). If YOU are awake much of the night…perhaps you need a screening for a sleep breathing disorder! A variety of symptoms can present when children/teens don’t get the proper quantity and quality of sleep regularly. Children […]

Is Your Child Oxygen Deprived? mouth breathing and the ramifications
If you find your child mouth breathing most of the time while sleeping or when sitting quietly, they have been oxygen deprived. Humans are typically the only “animals” that routinely breathe through the mouth instead of the nose. Watch your pets or animals; unless they just finished a bolt of running, they breathe through the […]




