We sleep about 1/3rd of our lives and science still can’t find a reason why we do. It’s such a fascinating cascade of chemistry, feedback loops and brain activity that still baffles science. There are still mysteries that our Creator uses to prove this stuff couldn’t just evolve. Sleep is one of those mysteries. Look […]

Can gum disease be contributing factor in Dementia and Alzheimer’s disease?
Increasing research is saying “YES”. Some of the aggressive Spirochetes that are found in patients “infected gums” are also found in the central nervous systems (Brain) of patients with Alzheimer’s and dementia. These spirochetes can “hide” from your immune system once inside the brain and may not show up as an infection or cause a […]

It’s Just Snoring
While many people do snore, heavy or severe snoring isn’t part of a healthy sleep pattern. Snoring is a sign that you’re not getting enough air with each breath. Pauses in breathing mean that your airway has closed. This is Obstructive Sleep Apnea. Snoring can also be a symptom of a serious health condition like […]
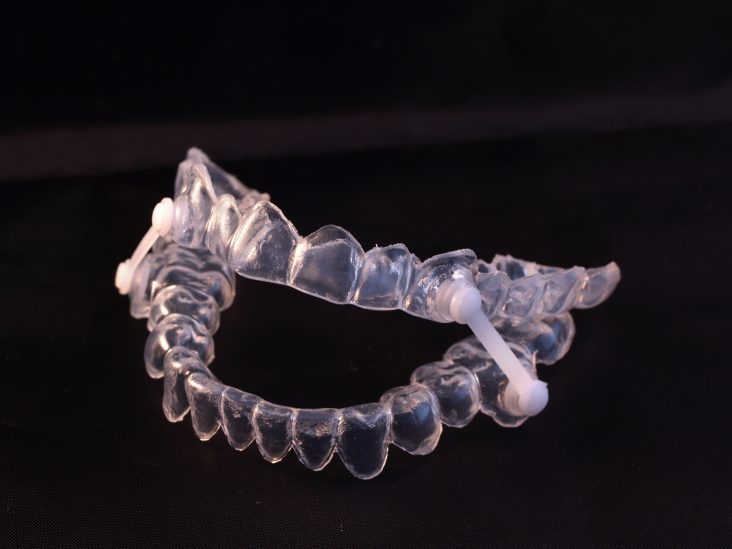
9 Tips on Oral Appliance Care
Custom and highly specific orthotic appliances are provided for differing TMD conditions and offer an alternative to CPAP for patients suffering from snoring and Sleep Breathing Disorders. These care instructions apply to all oral appliances, including night guards that may have been provided for clenching and grinding (bruxism). Store in case provided when not in use. […]

The Clench and Grind: Bruxism
There are known relationships between sleep disordered breathing, TMJ damage/dysfunction and clenching or grinding. In the dental industry, clenching and grinding is known as bruxing or bruxism. Because there are varying predispositions to bruxism and inconsistencies in the characteristics of subjects studied, the topic has been controversial in medical and dental journals in the past. […]

Use of Antibiotics for TMJ Arthritis?
Damage to the TMJ ligaments and disc results in joint sounds in most people. Clicking, popping, or grinding noises in the jaw joints (TMJ) indicates that ligaments have torn and the cartilage “disc” is being damaged and isn’t protecting the condyle. Eventually the popping and clicking “goes away” when the joint is rubbing “bone on […]

Sleep Apnea Diagnosis and Therapy
Sleep Apnea is becoming more prevalent and has been estimated to affect 1/3 of the adult population[i]. In our practice and in general literature, children have a high percentage of Sleep Breathing Disorders which leads to long term facial distortion, TMJ problems, malocclusion, and potential medical problems such as diabetes, obesity, impaired learning. Dentistry, and […]

Why might I need a sleep study and how do I get one?
A sleep study would be indicated by consistent snoring, feeling unrested after a night’s sleep (frequently), clenching or grinding of the teeth (indicates a high probability of a sleep breathing disorder), or repeated waking throughout the night. Any treatment a Dentist might provide to diagnose or treat a sleep breathing problem, needs the patient’s physician […]
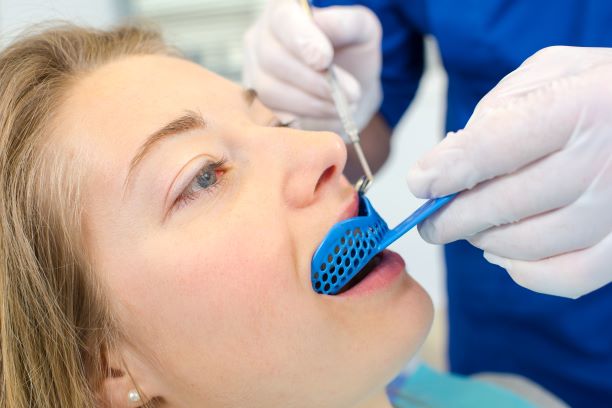
Using earplugs to decrease gagging during dental impressions?
Many people have a heightened gag reflex due to many different reasons, making dental treatment difficult. For those “easy gaggers” and others, the thought of having Dental Impressions of the teeth is stressful because it can stimulate the gag reflex. This reflex is called Arnolds Reflex, named after Freidrich Arnold, an anatomy physician in Germany […]

Licorice instead of flossing?
As we learn more about the benefits of “nature’s medicines” that other cultures use successfully for some conditions, it makes sense to give a few a serious look due to the lack of side effects that most prescription drugs have. It’s widely reported that oral diseases such as decay, gum disease, abscessed teeth, etc. are […]




